Why this blog?
Behind every delay, denial, or missed follow-up is a broken workflow. This blog shows how augmented intelligence can fix those gaps, making healthcare systems faster, safer, and more adaptive. It’s not about more AI tools, it’s about AI that fits where care happens.
By 2026, more than 80% of healthcare organizations will be using AI in their clinical and operational workflows. Already, adoption is rising fast, 66% of physicians used AI in 2024, up from just 38% in 2023. But here’s the catch, according to Gartner, fewer than 1 in 5 (20%) will see lasting results. The difference between success and disappointment isn’t the AI itself, it’s how well it fits into the workflow.
Augmented intelligence is quietly changing how care happens, not by overhauling workflows, but by weaving itself into them. It’s not the flashy kind of AI that makes headlines with robotic surgeries. It’s the kind that reshapes decisions in the background, at the nurse’s station, in billing queues, during a discharge call on a Friday evening.
That shift is well underway, but still poorly understood. While many see AI as a technology initiative, the organizations actually seeing impact have embraced it as a strategic redesign of how intelligence flows through their systems. This isn’t about models, it’s about operational memory, contextual adaptation, and human-computer co-reasoning. Augmented intelligence doesn’t replace your team. It changes what they’re capable of in real time.

Augmented Precision at the Point of Care
In high-volume clinical settings, every second is a resource and every click, a cost.
Consider a general hospital where physicians spend nearly half their day on documentation. Introducing GenAI-driven summarization here doesn’t just save time, it shifts how decisions get made. Among physicians who participated in a recent AMA (American Medical Association) survey, 57 % said that addressing administrative burdens through automation remains the biggest area of opportunity for AI. A discharge note that once took 15 minutes now takes 3. But more importantly, it’s contextually compressed, prioritizing actionable insights over raw transcription. Add auto-coded ICD tags, and downstream billing accuracy improves as well.
What are some of the measurable impacts seen by Healthcare institutions who have implemented augmented intelligence in their workflows?
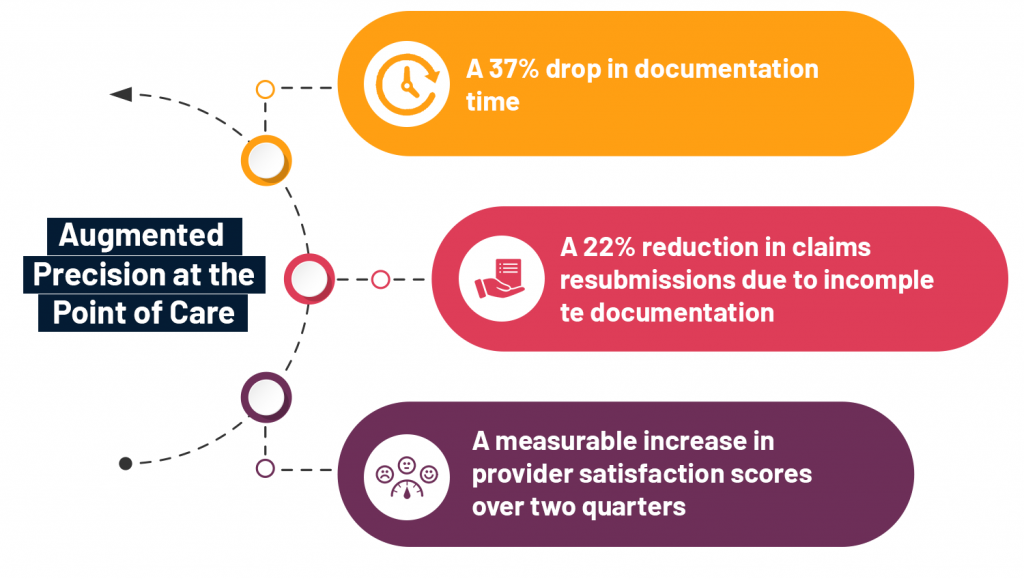
In a recent tertiary care deployment, this kind of GenAI augmentation led to:
- A 37% drop in documentation time
- A 22% reduction in claims resubmissions due to incomplete documentation
- A measurable increase in provider satisfaction scores over two quarters
A measurable increase in provider satisfaction scores over two quarters
Reducing Administrative Complexity Through Workflow-Aware AI
The hospital back-office is full of quiet inefficiencies: prior authorization queues, claim denials, repetitive data entry. These aren’t headline-grabbing pain points, but they’re exactly where augmented intelligence shines.
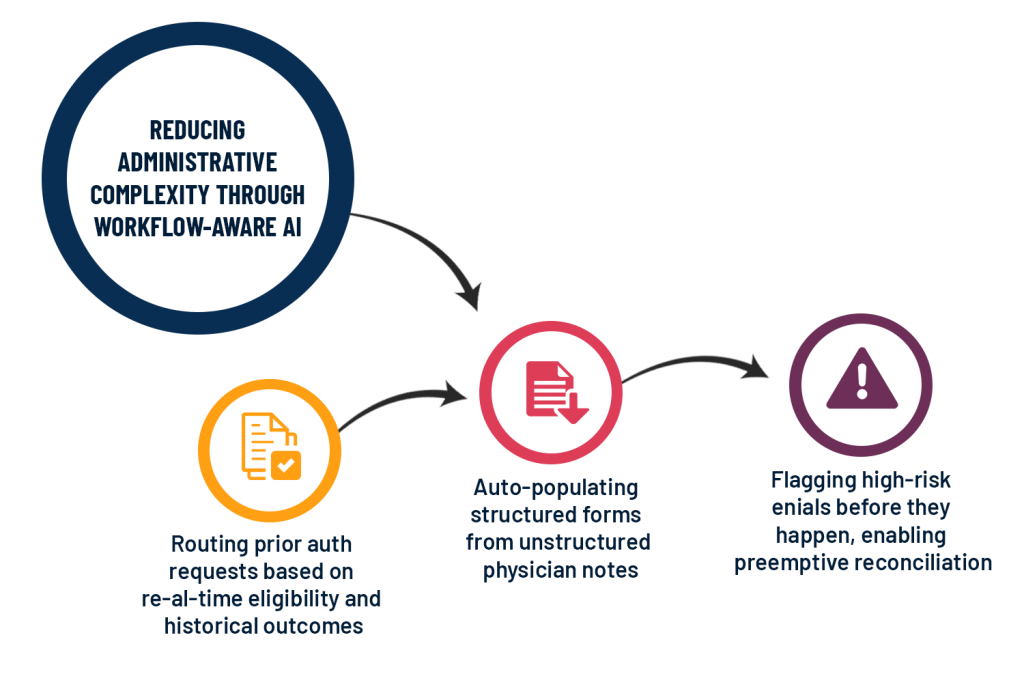
This orchestration layer doesn’t automate blindly. It learns the local rules, payer-specific patterns, compliance nuances, internal thresholds. And when done right, it augments teams rather than de-skills them.
In one multispecialty network, integrating augmented intelligence into the RCM workflow cut first-pass denials by 19% and improved average claim velocity by over 11 business days, without adding headcount.
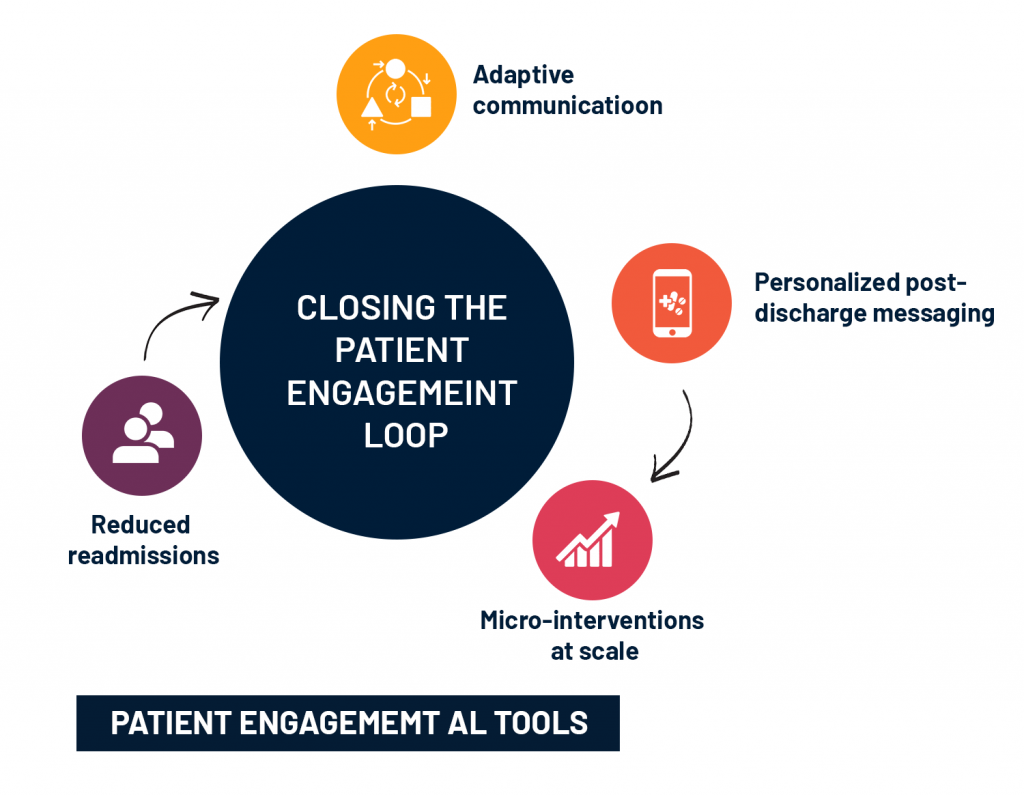
Closing the Loop in Patient Engagement
Engagement isn’t about apps or portals. It’s about understanding the patient’s moment, what they need, how they process information, and when they’re likely to act.
This is where augmented intelligence becomes human.
Instead of generic post-discharge texts, some systems are deploying GenAI bots that speak in the patient’s language (literally and emotionally), tuned to their recovery trajectory, comorbidities, and even preferred communication cadence. These aren’t dumb sequences,. they’re interaction models trained on hundreds of thousands of outcomes.
The results? Let us look at a case study that Factspan partnered with recently, a major U.S. health system saw a 25% lift in medication adherence and a 17% drop in unnecessary readmissions in pilot units using this adaptive communication model. These aren’t gimmicks, they’re micro-interventions, scaled. And on the provider side, it eliminates the burden of scripting, translating, or repeating the same compliance talk to every patient.
Closing the Gap Between AI Potential and Real-World Impact
Most augmented intelligence projects don’t fail because the models are bad, they fail because they’re dropped into the system like foreign objects. No integration into clinical pathways. No data harmonization. No behavioral design.
This is why the choice of partner is not a technical decision, it’s strategic.

And perhaps most importantly, they don’t treat implementation as an end state. They stay to tune, retrain, and re-align because in healthcare, real intelligence evolves.
Augmented Intelligence as the New Operating System of Care
Healthcare isn’t just a business of data. It’s a business of decisions made under pressure, often with imperfect information and human lives on the line. That’s why augmented intelligence matters, not because it automates, but because it amplifies. It elevates the judgment of a physician, the instincts of a nurse, the prioritization skills of a care coordinator.
In the next wave of digital transformation, the organizations that succeed won’t be the ones with the most AI tools. They’ll be the ones that think differently about intelligence, where it belongs, how it moves, and what kind of support it needs to make healthcare safer, faster, and more human.
The shift is already underway. Those who treat augmented intelligence not as a plug-in, but as an operating principle, will build systems that are not just smart but resilient, adaptive, and enduring.
And as patients, caregivers, and clinicians alike begin to trust those systems more, the impact won’t be in the code. It’ll be in the care.
Ready to see how augmented intelligence can reshape care delivery?

